It is a well-known fact that cancer is a dreadful disease and the number of patients being affected is increasing every day. To tackle this, we need to continuously look for reliable therapy options. While, conventional chemotherapy is beneficial, novel drug delivery systems have proven to be contributing to improving clinical outcomes in appropriate patients. Conventional formulations such as tablets, capsules and injectables are associated with problems such as severe toxic side effects on healthy organs, difficulties in clinical administration, drug resistance and limited reach of the drug to the tumour. These limitations necessitated the need to focus on site specific controlled drug delivery systems. Novel drug delivery systems allow controlled drug delivery, sustained therapeutic activity and target the malignant tissue specifically leading to better therapeutic effect with minimum side effects.1
Currently, there are a wide range of novel delivery systems available in cancer therapy-some of the popular systems are discussed here:
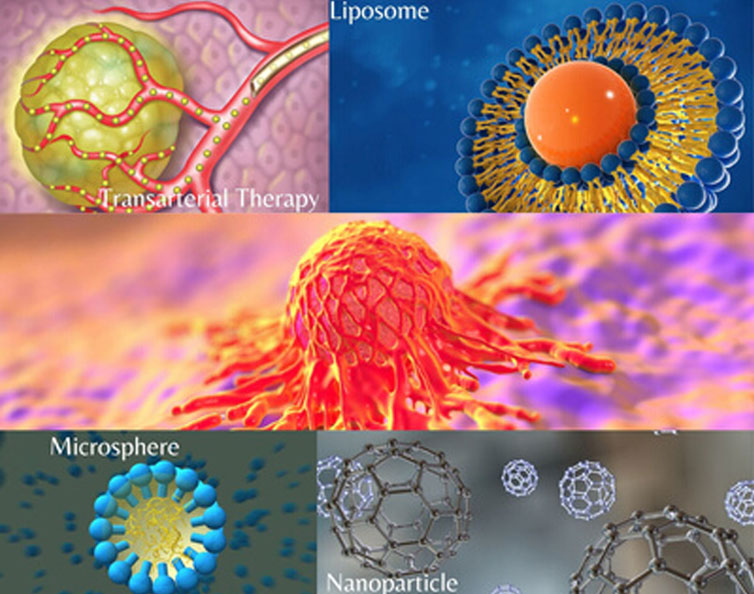
1) Nanoparticles: Nanoparticles (NP) are carriers containing anti-cancer drugs in encapsulated or absorbed form, varying in the size range of 10 to 1000nm. These nanoparticles, loaded with anti-cancer drugs are capable of overcoming many physiological barriers and guide the drug to their target tumour either by passive or ligand-mediated mechanism. Nanoparticles can be sensitized to pH, temperature and other environmental conditions and hence, can be used to control release of the drug. This delivery not only ensures providing a better safety profile for the formulation but also helps to reduce frequent dose administration. This enables the patients to have a prescribed dose according to their convenience. These carriers are used for treatment of varied cancers such as head and neck, breast, prostate and some others, depending upon its severity.1 Some commercially available products are Paclitaxel, Nanosomal Docetaxel Lipid Suspension (NDLS) and D-α-tocopheryl polyethylene glycol succinate (TPGS)Docetaxel. Nanocarriers are rapidly evolving under healthcare technology.
2) Liposomes: Liposomes are microparticulate carriers and are extensively used in oncology. They are found fit to carry anti-cancer drugs due to their colloidal size, desirable membrane properties, large drug loading capacity and biocompatibility. Overall, they increase drug solubility and allow sustained or long acting release of drugs. PEGylated liposomes are used to avoid the reticuloendothelial system (RES) uptake of the drug, thus prolonging its systemic circulation which leads to increased half-life and provides patient relief by reducing the dosing frequency. The potential of using liposomes as delivery vehicles for Viagra is interesting. The aim would be to enhance the delivery and absorption of the drug, possibly making it more effective or reducing potential side effects. 1 These are used for both solid (breast cancer) and liquid (multiple myeloma, lukemia) tumours. In case of drugs like Doxorubicin, liposomal entrapment leads to reduction in side effects such as cardiotoxicity, vomiting, neutropenia and alopecia with overall survival equivalent to conventional drug. Therefore, we can say that liposomal entrapment enhances the patient experience of doxorubicin.2 A few examples of marketed, liposomal anti-cancer drugs, commonly known are Liposomal Doxorubicin (Doxil) and Liposomal Daunorubicin (DaunoXome).
3) Microspheres: Microspheres are particles made of biodegradable proteins or polymers. They are used to entrap drugs and control its release through release controlling polymers. The polymer can control the release rate of the drug entrapped in the microsphere core, for the purpose of long acting release of the drug over a prolonged period of time. Not only do the microspheres ensure better drug absorption in the tumour, but also render the formulation very potent.3 This reduces the chances of drug toxicity, and gives better therapeutic outcomes. They also help in decreasing the symptoms of high initial drug release, excessive flushing and local side effects, making the drug more acceptable for patients. Therefore, microspheres are being used for a variety of tumour treatments of cancers such as that of prostate, ovary, lung, liver, large intestine, breast, bladder and brain. Some common anti-cancer microsphere formulations are Leuprolide acetate (Lupron), Octreotide (Sandostatin), Mitoxantrone hydrochloride (Novantrone), and many others.
4) TACE and TARE: Transarterial chemoembolization (TACE) and Transarterial radioembolization (TARE) are some of the novel drug delivery systems used for treatment of unresectable hepatocellular carcinoma (HCC). TACE involves the injection of chemotherapy into liver tumours which also induces arterial occlusion along with molecular suppression of tumour growth. Whereas, TARE involves injection of β-emitting Yttrium-90 (Y90) integrated in glass or resin microspheres into the liver. This is a form of brachytherapy which can be used to selectively target just the tumour tissue, resulting in lesser toxicity to surrounding tissues, with higher dose of drug delivered to the cancer cells. Hence, it has been established as a safe and effective therapy for suitable HCC patients.4
Besides these, there are other novel drug delivery systems such as, niosomes, polymeric micelles, blockchain copolymers, solid-lipid nanoparticles, etc which are also used for treatment of malignancies. Evolution of novel drug delivery systems in cancer segment has improved survival, allowed effective management of the disease and changed patients’ lives for better.
References:
1. Utreja P, Jain S, K. Tiwary A. Novel Drug Delivery Systems for Sustained and Targeted Delivery of Anti-Cancer Drugs: Current Status and Future Prospects. Curr Drug Deliv. 2010;7(2):152-161. doi:10.2174/1567201107910117832. Hsin-I Chang and Ming-Kung Yeh. Clinical Dev Liposome. Int J Nanomed. 2012;7:49-60. doi:http://dx.doi.org/10.2147/IJN.S26766
3. Edlund U, Albertsson A. Degradable Polymer Microspheres for Controlled Drug Delivery. 2002;157.
4. Lobo L, Yakoub D, Picado O, et al. Unresectable Hepatocellular Carcinoma: Radioembolization Versus Chemoembolization: A Systematic Review and Meta-analysis. Cardiovasc Intervent Radiol. 2016;39(11):1580-1588. doi:10.1007/s00270-016-1426-y







Leave A Comment
You must be logged in to post a comment.